Introduction
Attention-Deficit/Hyperactivity Disorder (ADHD) is a common neurodevelopmental condition known for symptoms of inattention, hyperactivity, and impulsivity. Many patients and families ask whether ADHD can cause anxiety or depression. The short answer: ADHD doesn’t directly cause anxiety disorders or depressive disorders, but it can significantly increase the risk of developing them. In fact, ADHD often co-occurs with anxiety and depression – a phenomenon known as comorbidity. Understanding the link between ADHD and these conditions is important for effective treatment. This comprehensive article explores whether anxiety or depression are symptoms of ADHD, separate diagnoses, or possible outcomes of unmanaged ADHD. We’ll also discuss current clinical research on ADHD with co-occurring anxiety/depression, and treatment guidelines to help patients manage these challenges.
Medically Reviewed By:
Dr. Irfan Akram, MD
Board-Certified Psychiatrist | ADHD Specialist | Comprehensive Psychiatry – Reston, Virginia
Serving Virginia, Maryland, and Washington DC.
What Is ADHD?
ADHD is a developmental brain-based disorder characterized by persistent patterns of inattention (e.g. difficulty focusing, disorganization) and/or hyperactivity-impulsivity (e.g. restlessness, fidgeting, acting without thinking). Symptoms begin in childhood and often continue into adulthood. ADHD can make it hard to stay organized, meet deadlines, and control impulses. It’s not classified as a mood disorder or an anxiety disorder – it’s in its own category. However, ADHD often co-occurs with other mental health conditions. The National Institute of Mental Health notes that ADHD frequently co-occurs with anxiety or depression, among other conditions, which can make diagnosis and treatment more complex. In other words, while ADHD itself has specific core symptoms, a person with ADHD might also experience separate issues like chronic worry or prolonged sadness that suggest an additional diagnosis.
Importantly, anxiety and depression are not part of the diagnostic criteria for ADHD. If someone with ADHD has symptoms like constant anxious thoughts or persistent depressed mood, these typically indicate a separate anxiety disorder or depressive disorder occurring alongside ADHD, rather than ADHD itself. That said, living with unmanaged ADHD can take an emotional toll. Struggling in school or work, receiving frequent criticism, or feeling different from peers can lead to frustration and low self-esteem. Over time, these stressors can contribute to the development of anxiety or depression. To understand this better, let’s examine ADHD’s relationship with anxiety and with depression in turn.
The Link Between ADHD and Anxiety
Many individuals with ADHD also experience significant anxiety. Research shows that roughly 30–50% of people with ADHD will also have an anxiety disorder in their lifetime. This rate is much higher than in the general population, indicating a strong link. Does this mean ADHD causes anxiety? Not exactly – but ADHD can set the stage for anxiety to flourish.
ADHD and anxiety often occur together due to a mix of overlapping symptoms, shared biology, and life experiences. On a biological level, some of the brain pathways involved in ADHD (such as those regulating attention and impulsivity) overlap with pathways that regulate anxiety and fear responses. For example, both conditions have been linked to differences in dopamine and other neurotransmitters in the frontal lobe of the brain. This means a person’s genetic makeup or brain chemistry could predispose them to both ADHD and anxiety independently. In such cases, one condition isn’t directly causing the other – instead, the same underlying biology contributes to both.
There are also psychological and lifestyle factors. ADHD symptoms – like chronic procrastination, disorganization, forgetfulness, or impulsivity – can lead to stressful situations. A student with ADHD might miss assignment deadlines or a professional might struggle with punctuality and project completion. These ongoing challenges often result in chronic stress, social criticism, and a feeling of being overwhelmed. Over time, chronic stress can evolve into generalized anxiety disorder or other anxiety disorders. For instance, someone with untreated ADHD may worry constantly about forgetting tasks or making mistakes at work, eventually developing clinically significant anxiety in addition to their ADHD. In this way, unmanaged ADHD can indirectly cause anxiety by creating life circumstances that provoke excessive worry.
It’s also worth noting that some symptoms overlap between ADHD and anxiety, which can blur the lines. Both conditions can involve restlessness, difficulty concentrating, and even sleep problems. A person with ADHD might say “I can’t focus because my mind jumps around,” whereas a person with anxiety might say “I can’t focus because I’m consumed by worries.” The outward complaint (trouble focusing) is similar, but the root cause is different. Professionals often find that distinguishing ADHD from anxiety requires careful evaluation. As one clinician explains, when a patient reports concentration problems, the cause could be ADHD’s executive function deficits, anxiety’s constant worry, or even depressive fatigue. Each requires a different treatment approach.
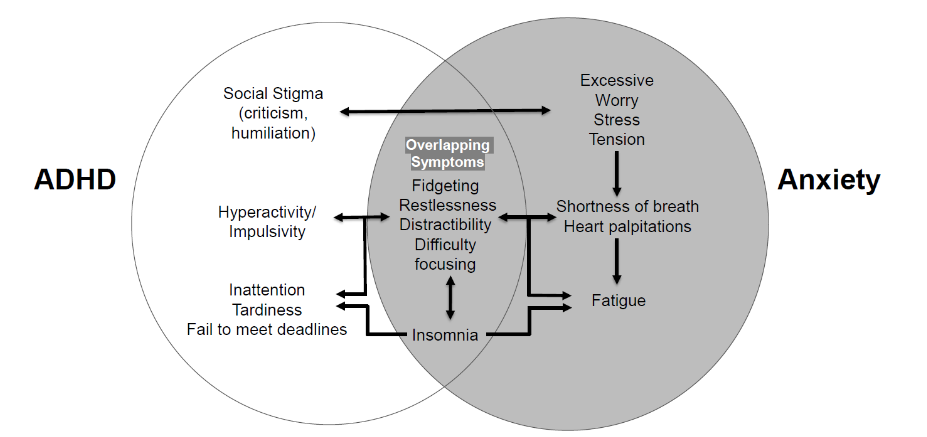
Understanding overlapping symptoms of ADHD and anxiety. Many symptoms – such as restlessness, insomnia, or difficulty concentrating – can appear in both ADHD and anxiety disorders. However, the underlying causes differ: ADHD may lead to missed deadlines and social stigma (left circle), fueling worry, while anxiety involves excessive fear and tension (right circle). The overlapping area shows common symptoms like fidgeting and distractibility that can stem from either or both conditions.
ADHD and Anxiety: Comorbidity vs. Causation
Experts consider ADHD with co-occurring anxiety as comorbid conditions rather than a straightforward cause-and-effect relationship. Long-term studies find that ADHD and anxiety are independently expressed – meaning each condition follows its own course, though they influence each other. For example, some children with ADHD might never develop significant anxiety, especially if their ADHD is well-managed and their environment is supportive. Others might develop an anxiety disorder due to challenges faced by ADHD. Interestingly, when ADHD and anxiety coexist, the combination can alter how symptoms present. Some research suggests that anxiety in ADHD may actually temper certain ADHD behaviors (for instance, a person might become less impulsive because they’re more worried and cautious) but at the same time anxiety can worsen other issues like working memory and focus. The net result is often that having both conditions makes daily life even harder than having either one alone.
The key takeaway is that ADHD increases the likelihood of anxiety but usually doesn’t directly cause an anxiety disorder in the way a virus causes an illness. If you have ADHD and also feel constant worry, nervousness, or panic, it’s important to recognize these as signs of a possible separate anxiety disorder that warrants attention. Approximately 50% of adults with ADHD also experience an anxiety disorder at some point, so you are not alone – and effective treatments exist to manage both conditions.
Can ADHD Cause Depression?
Just as with anxiety, ADHD is associated with a higher risk of depression. Adults with ADHD are several times more likely to experience major depressive disorder in their lifetime compared to those without ADHD. Estimates vary, but roughly 30% (or more) of people with ADHD will have a depressive episode during their life. In youths, studies have found rates of major depression in kids/teens with ADHD ranging from about 12% up to 50%, which is five times higher than in those without ADHD. Clearly, there is a notable link.
Does that mean ADHD causes depression? Again, not in a direct biological sense – ADHD and depression are classified as distinct disorders. However, ADHD’s impact on life can lead to circumstances that trigger depression. Think about the classic symptoms of depression: persistent sadness, low self-esteem, feelings of guilt or worthlessness, loss of interest in activities, and hopelessness. Now consider a person with ADHD who, despite trying hard, keeps falling short of expectations: poor grades despite being smart, repeated job losses due to disorganization, strained relationships from impulsive remarks, etc. Over years, these repeated frustrations and failures can cause a person to feel demoralized and hopeless. In fact, some researchers refer to “ADHD-related demoralization” – the idea that the impairments and negative experiences from unmanaged ADHD can lead to a true depressive disorder. The individual might start believing “I’ll never be able to do anything right,” which can spiral into clinical depression.
It’s critical to understand that when someone with ADHD becomes depressed, it is not just a character flaw or inevitable outcome, but a co-occurring condition that should be properly treated. While the depression may be secondary to the ADHD in terms of what appeared first, it is a real depression with its own set of symptoms and risks (and not merely sadness due to ADHD setbacks). In other words, ADHD and depression have independent courses; having ADHD doesn’t mean you are destined to be depressed, but it does raise the risk and often the depression, if it occurs, needs to be addressed as its own problem.
To answer the question plainly: ADHD itself does not inherently include depression as a symptom, but the challenges of ADHD can lead to depression over time. Many adults with lifelong ADHD report that untreated symptoms led to chronic stress and negative self-image, culminating in depression in adulthood if support wasn’t provided early. The silver lining is that recognizing this pattern means we can intervene – by treating the ADHD effectively and providing support (academic accommodations, therapy, coaching) to prevent that downward spiral into depression.
ADHD and Depression: Signs to Watch
How can you tell if someone’s sadness is related to ADHD or is a separate depression? It can be tricky, since some symptoms overlap. For instance, low motivation and lack of focus can be signs of both ADHD and depression. One clue is timing: ADHD is typically present from childhood, whereas depression might develop later. If a person with ADHD has been relatively stable mood-wise but then experiences a period of persistent sadness, hopelessness, or loss of interest that lasts weeks or months, it could signal a depressive episode on top of their ADHD. Clinicians will often ask whether the individual’s difficulties with concentration or motivation got significantly worse at a certain point (suggesting depression), or whether those issues have always been there (more consistent with just ADHD). Research indicates that depressive disorders in people with ADHD usually occur several years after the onset of ADHD symptoms. So if you have ADHD and start feeling depressive symptoms in your teens or adulthood, it’s likely a coexisting depression rather than an inherent part of ADHD.
Also, the emotional tone differs: ADHD can cause frustration and momentary disappointment, but clinical depression brings a pervasive sadness or emptiness that doesn’t lift, even when circumstances change. People with ADHD often have fluctuating emotions (upset when an immediate problem occurs, but quick to recover with a solution or support). In contrast, depression’s gloom is more persistent and disproportionate to any one trigger. If you or your loved one with ADHD experiences symptoms like intense sadness, frequent crying, withdrawal from friends, feelings of worthlessness, or any thoughts of self-harm, those are not simply “ADHD mood swings” – they are red flags of depression that should be addressed promptly.
Are Anxiety and Depression Symptoms of ADHD, or Separate Diagnoses?
To summarize the distinction: Anxiety and depression are separate diagnoses, not symptoms of ADHD. ADHD has a specific symptom profile (inattention and/or hyperactive-impulsive symptoms). Anxiety disorders (like generalized anxiety, social anxiety, panic disorder) have their own hallmark symptoms such as excessive worry, fear, and physical anxiety symptoms (racing heart, sweating). Depression (major depressive disorder) is characterized by persistent low mood, loss of pleasure, changes in sleep/appetite, etc. These are not part of ADHD’s definition. However, ADHD frequently coexists with these conditions. Coexistence (comorbidity) means a person meets criteria for two or more disorders at the same time.
Why is this important? Because if anxiety or depression is present alongside ADHD, it should be recognized and treated in its own right. One study from the National Comorbidity Survey found that individuals with ADHD are three times more likely to develop a mood disorder like depression compared to people without ADHD. Similarly, other research has noted that adults with ADHD have a higher chance of various anxiety disorders. In practice, about 70% of adults with ADHD will have at least one other psychiatric disorder over their lifetime – often an anxiety or mood disorder. So if you only treat the ADHD but ignore the anxiety/depression, the person may continue to suffer. Conversely, misattributing everything to ADHD when someone is actually anxious or depressed could lead to incomplete treatment.
It’s also worth noting that ADHD can involve emotional dysregulation (difficulty managing emotions, quick frustration or excitement), which is not the same as an anxiety disorder or depressive disorder. For example, a child with ADHD might have temper outbursts or feel discouraged by setbacks – but these tend to be situation-specific and improve when the ADHD is managed (structure, behavioral therapy, medication, etc.). If the child has an actual anxiety disorder, they will exhibit excessive worry in many situations, even when things are going well. If they have a depressive disorder, the low mood and lack of enjoyment persist even when positive events happen. This distinction can be nuanced, which is why a thorough evaluation is crucial.
Impact of Comorbidity on Daily Life
When ADHD and anxiety or depression occur together, the impact on daily functioning is often greater than either condition alone. Comorbidity can create a vicious cycle: ADHD symptoms (like disorganization or impulsivity) can lead to stressful outcomes that fuel anxiety/depression, and in turn anxious or depressive symptoms (like constant worry or low energy) can worsen ADHD by making it even harder to concentrate or stick to routines. For example, an adult with ADHD might struggle with forgetfulness and miss a work deadline, leading to anxiety about job security; that anxiety then causes insomnia, which the next day makes their ADHD symptoms (inattention, irritability) worse, potentially leading to more mistakes – and the cycle continues. Similarly, a teen with ADHD might feel so demoralized by academic failures that they develop depression; that depression saps their motivation to even try, so their school performance further declines.
Research underscores that comorbid conditions intensify the burden of illness. Those with both ADHD and depression tend to have more severe depressive episodes and longer durations of illness than people with depression alone. Quality of life, academic and work success, and self-esteem are often lower in people who have ADHD plus anxiety/depression compared to those with just one of these conditions. It’s not hard to see why: juggling the impulsivity and concentration problems of ADHD alongside the hopelessness of depression or the dread of anxiety can be overwhelming. This is why clinicians stress treating all co-occurring conditions, not just one. A comprehensive approach gives the best chance of a good outcome.
The good news is that with integrated treatment and support, individuals with ADHD and comorbid anxiety/depression can and do improve. Many find that when their ADHD is properly managed (with strategies, accommodations, or medication), they gain confidence and control in their life, which in turn reduces anxiety and boosts mood. Likewise, addressing anxiety or depression with therapy or appropriate medication can provide emotional relief that allows the person to make better use of ADHD management strategies. Let’s look next at how professionals diagnose and treat these co-occurring conditions.
Diagnosis and Treatment of ADHD with Comorbid Anxiety/Depression
Diagnosing coexistent ADHD and anxiety/depression requires a careful assessment by a qualified mental health professional (such as a psychiatrist or clinical psychologist). The evaluator will take a thorough history – asking about the timeline of symptoms, contexts in which they occur, and family history. As mentioned, one telling factor is the timing of symptom onset. ADHD starts in childhood (symptoms generally present before age 12, even if a person wasn’t diagnosed until later). Anxiety and depression can arise at any age, often in adolescence or adulthood. If an adult reports they never had attention problems in childhood but are now very unfocused after a period of extreme stress or sadness, the clinician might consider that the concentration issue is secondary to an adult-onset anxiety or depression, rather than true ADHD. On the other hand, if someone has lifelong ADHD and then develops chronic anxiety in college, it likely means they have both ADHD and an anxiety disorder. Skilled clinicians use standardized rating scales and diagnostic interviews to tease these apart. Sometimes it’s necessary to treat one condition first and see what symptoms remain, to clarify the diagnosis.
When it comes to treatment, a multi-pronged approach is often best. There is no single medication or therapy that fixes ADHD, anxiety, and depression all at once, but we have effective treatments for each, and they can be combined safely. Medication is a cornerstone for moderate to severe cases of ADHD and/or depression/anxiety:
For anxiety and depression, antidepressant medications (particularly Selective Serotonin Reuptake Inhibitors (SSRIs) or Selective Norepinephrine Reuptake Inhibitors (SNRIs)) are commonly used. These medications help rebalance brain chemistry to alleviate anxious worry and depressed mood. They do not treat ADHD symptoms, but they can greatly relieve the co-occurring anxiety or depression
For ADHD, stimulant medications (like methylphenidate or amphetamine-based meds) or certain non-stimulants (like atomoxetine or guanfacine) are first-line treatments. These medications significantly improve focus, impulse control, and organization in most individuals with ADHD.
In patients who have both ADHD and depression, doctors often prescribe both a stimulant and an antidepressant, and studies have shown this combination to be safe and effective. For example, someone might take a stimulant in the morning for ADHD and an SSRI in the evening for anxiety/depression. There isn’t generally a contraindication to using ADHD medications alongside antidepressants, though the timing of introducing them might be staggered. In some cases, if it’s unclear which condition is “driving” the other, a doctor may start by treating the condition that is causing the most impairment at the moment. One common strategy with adults is to treat the ADHD first – since stimulants work quickly (often within days) – and then see how the patient is doing. If a lot of the anxiety or low mood was stemming from ADHD chaos, improving the ADHD may automatically lessen the anxiety/depressive symptoms. If significant anxiety or depression remains even after ADHD is well-controlled, then adding therapy or an antidepressant for those symptoms makes sense.
In some situations, particularly where anxiety is very prominent, doctors might choose a non-stimulant ADHD medication like atomoxetine, which can treat ADHD symptoms and has some anxiety-reducing effect. Atomoxetine is a non-stimulant that boosts norepinephrine and has been found to help ADHD patients with comorbid anxiety without worsening the anxiety – in fact, one study showed it could reduce anxiety symptoms while treating ADHD. This can be a great option if stimulants prove too activating for a given patient or if there’s a coexisting substance abuse concern that makes stimulants risky.
Therapy and Behavioral Interventions are equally important. For anxiety and depression, Cognitive Behavioral Therapy (CBT) has a strong evidence base. CBT helps individuals challenge unhelpful thoughts (like catastrophizing or negative self-talk) and develop coping strategies for stress and low mood. In the context of ADHD, therapy might also focus on organizational skills, time management, and coping mechanisms for ADHD symptoms (sometimes called ADHD coaching or therapy). In fact, combining medication for ADHD with therapy for anxiety/depression yields a one-two punch: medication improves the neurochemical balance, while therapy equips the patient with psychological tools. Family therapy or parent training can help when dealing with children or teens, so that family members learn how to support the child’s needs without inadvertently increasing pressure or negativity.
Lifestyle adjustments are valuable too. Exercise, sleep, and structure are three big ones:
- Regular exercise has been shown to improve mood and anxiety, and even helps increase focus for those with ADHD.
- Ensuring consistent, adequate sleep is vital because sleep deprivation can worsen both ADHD symptoms and emotional regulation. (Sometimes treating ADHD can improve sleep, as the racing thoughts at night diminish, and conversely, addressing anxiety can improve sleep which then aids focus.)
- Structured routines and external organization systems (planners, reminders) reduce the chaos that feeds anxiety/depression.
Lastly, support groups or psychoeducation for ADHD can reduce the sense of isolation and hopelessness. Learning about how ADHD affects your brain and hearing others’ success stories can transform demoralization into motivation and self-compassion.
When to Seek Help
If you or your family member has ADHD and you notice signs of significant anxiety or depression, it’s important to seek help rather than assuming it’s “just part of the ADHD.” Here are some cues that professional evaluation is needed:
- Persistent Anxiety: Feeling constantly on edge, worried, or panicky on most days, to the point it interferes with work, school, or enjoying life. For example, an adult with ADHD who cannot sleep due to racing worries or a child with ADHD who is terrified to go to school might be showing an anxiety disorder in need of treatment.
- Persistent Depression: Ongoing sadness, tearfulness, or irritability; loss of interest in hobbies; social withdrawal; or comments about feeling worthless or hopeless. Any talk of not wanting to live or other suicidal thoughts must be taken seriously and addressed immediately with professional help.
- Worsening of ADHD Functioning: If previously manageable ADHD symptoms have worsened because of constant worry or low mood, it’s a sign that a secondary condition might be present. For instance, perhaps you always had some trouble focusing, but now your motivation is so low that you’re missing work days – this could indicate depression on top of ADHD.
- Impact on Daily Life: Essentially, if anxiety or sadness is adding a new layer of impairment beyond what ADHD alone accounted for, don’t wait. Reaching out to a healthcare provider can clarify what’s going on.
Remember, effective help is available. Conditions like ADHD, anxiety, and depression are not character flaws or personal failures – they are medical issues that professionals can treat. Early intervention can prevent things from snowballing. For example, treating anxiety early may stop it from severely disrupting school or work, and addressing depression promptly can prevent months of suffering. If you’re unsure, consider having an evaluation; a mental health professional can differentiate whether it’s just ADHD or something more. It’s always better to ask than to ignore signs of distress.
How Comprehensive Psychiatry Can Help
Managing ADHD with co-occurring anxiety or depression can be challenging, but you don’t have to do it alone. Comprehensive Psychiatry, led by Dr. Imran Akram, MD, specializes in ADHD and related mental health conditions. Dr. Akram is a licensed, board-certified psychiatrist with over 15 years of experience helping patients navigate ADHD and its impact on mood and well-being. Our clinic, based in Reston, Virginia, serves patients across Virginia (VA), Maryland (MD), and Washington, DC – both in-person and via telepsychiatry – providing convenient access to care for those in the VA-MD-DC region.
At Comprehensive Psychiatry, we take an integrated approach to treatment. When a patient comes in with ADHD and anxiety and/or depression treatment, we perform a thorough assessment to understand all facets of their situation. We then create a personalized treatment plan that may include medication management for ADHD (e.g., stimulants or non-stimulants) and for anxiety/depression (e.g., SSRIs or other appropriate medications) as needed. Just as importantly, we emphasize psychotherapy and practical strategies: our team collaborates with therapists skilled in treating ADHD and anxiety or ADHD and depression combinations. This might involve cognitive-behavioral techniques, stress management training, or ADHD coaching to develop organizational skills. By addressing both the ADHD symptoms and the emotional symptoms, we aim to break the vicious cycle and help patients regain control of their lives.
If you’re looking for an experienced ADHD psychiatrist for treatment in Virginia who understands the nuanced link between ADHD and anxiety or depression, Dr. Akram offers the expertise and compassionate care you need. We also offer treatment for ADHD and anxiety in Maryland through accessible services for our Maryland patients, and likewise assist individuals in Washington, DC. No matter where you are in the DMV (DC-Maryland-Virginia) area, you can seek expert help to manage your symptoms and improve your quality of life. Our goal is not just to reduce symptoms, but to help you or your loved one thrive at school, work, and relationships by fully addressing all aspects of mental health.
Conclusion
While ADHD itself does not directly cause an anxiety disorder or depression, it often goes hand-in-hand with these conditions. The stresses and struggles of unmanaged ADHD can lead to significant anxiety or depressed mood over time, and biologically, having ADHD predisposes an individual to other mental health conditions. It’s more accurate to say ADHD and anxiety/depression are linked – frequently co-occurring and intertwined – rather than one simply causing the other. For patients and families, the important message is that anxiety and depression are not “just ADHD”; they are real, treatable conditions. Identifying them and getting comprehensive treatment can make a tremendous difference in outcomes.
Living with ADHD, anxiety, or depression can undoubtedly be challenging, especially if more than one is present. However, with proper care – including tailored strategies, therapy, and if appropriate, medication – individuals can manage their symptoms effectively. Many people with ADHD and comorbid anxiety/depression learn to leverage their strengths, overcome their challenges, and lead fulfilling, productive lives. The path may involve some trial and error in finding the right treatment balance, but improvement is very achievable.
If you or someone you love in Virginia, Maryland, or Washington, DC is struggling with ADHD and anxiety or depression, consider reaching out for professional help. Dr. Irfan Akram and the team at Comprehensive Psychiatry are here to provide compassionate, expert care. With the right support, you can address each aspect of your mental health and move toward a better quality of life. Remember, you are not alone, and getting help is a brave and important step.
Sources:
https://www.aafp.org/pubs/afp/issues/2012/0501/p890.html
https://esmed.org/comorbid-adhd-and-anxiety-treatment-prioritization-insights/
https://therapygroupdc.com/therapist-dc-blog/adhd-anxiety-and-depression-understanding-when-all-three-conditions-overlap/
https://www.nimh.nih.gov/health/topics/attention-deficit-hyperactivity-disorder-adhd
