Cognitive Behavioral Therapy in Reston Virginia
Trusted Psychiatric & mental health therapy in DMV Region
What Is Cognitive Behavioral Therapy?
Cognitive Behavioral Therapy (CBT) is a structured, evidence-based form of psychotherapy that helps individuals identify and change unhelpful thought patterns and behaviors that contribute to emotional distress.
CBT is based on a simple but powerful principle:
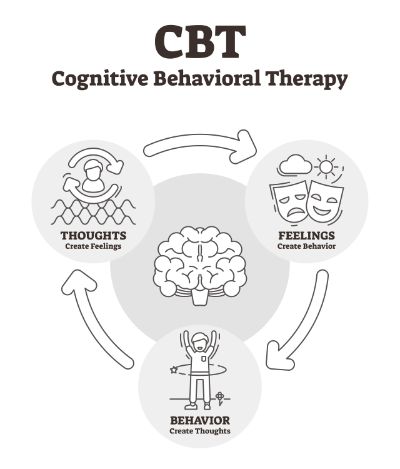
The way we think affects the way we feel, and the way we feel influences how we behave.
When negative thinking patterns become automatic, they can fuel anxiety, depression, trauma responses, and other psychiatric conditions. CBT works by breaking this cycle and replacing distorted thoughts with balanced, realistic ones.
Unlike long-term, insight-based therapies, CBT is:
- Goal-oriented
- Time-limited
- Skill-focused
- Collaborative
Patients actively participate in learning tools they can use for life.

How Does CBT Work?
CBT works by targeting three interconnected areas- Thoughts, Emotions and Behaviors.
Thoughts (Cognitions)
Identifying distorted thinking patterns such as catastrophizing, black-and-white thinking, overgeneralization, or mind reading.
Emotions
Understanding how these thoughts trigger emotional responses like anxiety, guilt, sadness, fear, or anger.
Behaviors
Modifying avoidance, withdrawal, compulsions, or other behavioral responses that reinforce distress.
Through guided sessions, patients learn how to:
This rewiring strengthens emotional regulation and psychological resilience.
What Conditions Is CBT Used For?
CBT is one of the most researched and widely recommended therapies in modern psychiatry. It is commonly used to treat:
Because of its structured and adaptable approach, CBT can be customized for adolescents, adults, and older adults.
Why Is CBT Considered Evidence-Based?
CBT is supported by decades of clinical research. It is frequently recommended by leading institutions including the National Institute of Mental Health and the American Psychological Association.
Research consistently shows that CBT:
- Reduces symptoms of anxiety and depression
- Lowers relapse rates in major depressive disorder
- Improves coping skills in trauma survivors
- Reduces compulsive behaviors in OCD
- Enhances long-term emotional stability
Many studies demonstrate that CBT can be as effective as medication for certain conditions, and often more effective when combined with medication under psychiatric supervision.
Cognitive Behavioral Therapy Common FAQs
What Happens During a CBT Session?
A typical CBT session includes:
- Review of current symptoms
- Identification of problematic thought patterns
- Cognitive restructuring exercises
- Behavioral strategy planning
- Skill-building assignments for real-life practice
Unlike passive talk therapy, CBT requires active participation. Patients often receive practical exercises or “homework” to reinforce skills between sessions.
Sessions are structured but supportive, focusing on real-life problem-solving.
How Long Does CBT Take?
CBT is generally short- to medium-term.
- Mild anxiety or stress: 6–8 sessions
- Moderate depression or anxiety: 12–20 sessions
- Complex trauma or OCD: longer, structured treatment plans
Progress depends on- Co-existing psychiatric conditions, Severity of symptoms, Consistency of attendance, Engagement in between-session exercises.
How Effective Is Cognitive Behavioral Therapy?
Effectiveness depends on the condition and patient participation. However:
- Anxiety disorders show strong improvement rates.
- Depression outcomes are comparable to antidepressant treatment in many cases.
- OCD and PTSD outcomes improve significantly with structured CBT protocols.
One of CBT’s biggest advantages is that it teaches lifelong coping tools- meaning benefits often continue even after therapy ends.
What Are the Benefits of CBT for Patients?
Patients after receiving CBT therapy from mental health specialists often report Improved emotional regulation, Better stress management, Reduced panic symptoms, Improved self-awareness, Stronger problem-solving skills, Increased confidence, and Decreased avoidance behaviors.
CBT empowers patients with practical tools rather than dependency on therapy alone.
Are There Any Side Effects or Risks?
CBT is considered safe and low-risk.
However, some individuals may initially experience:
- Temporary emotional discomfort when confronting fears
- Increased awareness of distressing thoughts
- Anxiety during exposure exercises
These reactions are usually short-term and part of the therapeutic process.
CBT does not involve medication and does not produce physiological side effects.
What Works Best With CBT?
CBT often works best when combined with Medication management (when appropriate), Lifestyle modifications (sleep, nutrition, exercise), Mindfulness technique, Family support, and Stress reduction strategies.
In psychiatric settings, CBT is frequently integrated into a comprehensive treatment plan.
What Changes in the Brain With CBT?
Research in neuropsychology suggests CBT may:
- Strengthen prefrontal cortex activity (decision-making and emotional regulation)
- Reduce overactivation in the amygdala (fear center)
- Improve neural pathways related to stress response
Over time, CBT supports healthier neural connections associated with resilience and emotional stability.
Who Is a Good Candidate for CBT/Who Needs CBT Therapy?
CBT may be ideal for individuals who are open to practicing skills outside sessions, prefer structured therapy, want practical coping strategies, struggle with negative thinking patterns, experience anxiety, depression, or trauma-related symptoms.
Why Choose CBT at a Psychiatric Clinic?
When CBT is offered within a psychiatric clinic:
- Therapy can be coordinated with medication management.
- Treatment plans are medically supervised.
- Co-occurring conditions are addressed comprehensively.
- Progress is tracked clinically.
This integrated approach improves long-term outcomes.